Looking for a tool that can help you assess a person's fall risk factor? Read our guide to learn more about the importance of assessing fall risk in patients who've suffered falls before, as well as those whose mobility has been negatively impacted by medical issues. Then, download the Morse Fall Scale to assess such patients.
## **The second leading cause of disability in the world**
The World Health Organization has deemed falls as the second leading cause of disability in the world (World Health Organization, 2021). Based on data they've accrued, they've determined that, globally, around 684,000 people die because of falls, with 80% of those coming from low and middle-income countries. They've also determined that adults 60 years and up are the ones who make up a good percentage of deaths due to falls.
There are many factors that contribute to a person's fall risk. Examples of such factors include having weak muscles (in general, but most especially in the legs), poor balancing, injuries from previous falls, injuries in the legs due to accidents, impaired mobility, dizziness, lightheadedness, confusion, cognitive impairment, having vision and hearing problems, being inebriated, and having certain diseases like diabetes, thyroid dysfunctions, arthritis, depression, etc. (NHS Inform, 2023) lead to increased risk of falling.
For medical professionals handling people with high fall risks, especially those with musculoskeletal or neurological problems, and those who are considered elderly (those aged 60+), it's important to routinely monitor such patients using tools that assess fall risk, one of which is the Morse Fall Scale.
## **What is the Morse Fall Scale?**
The Morse Fall Scale (MFS) is a tool healthcare providers use to assess an individual's fall risk. J. M. Morse developed it in the 1980s to help identify patients at high risk for falls and to help with developing interventions and plans for preventing falls.
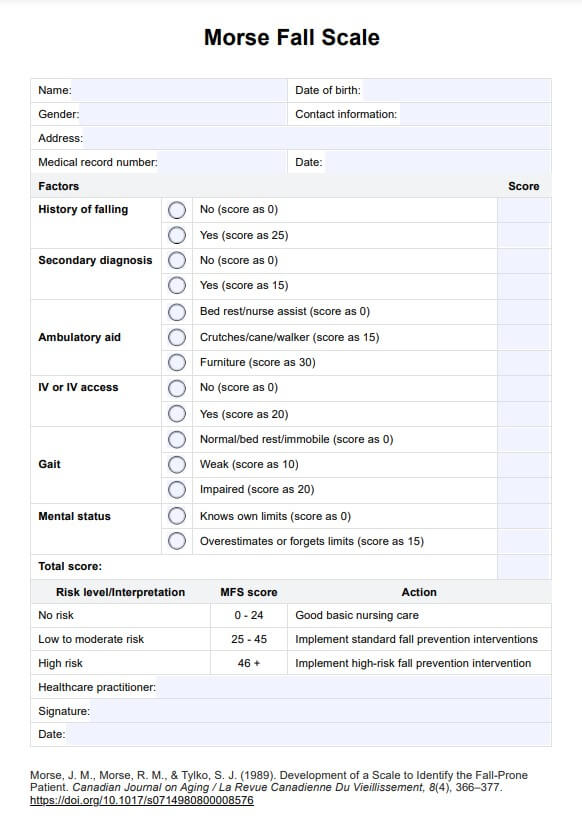
The scale comprises six categories assessed to determine an individual's fall risk (Morse, Morse, & Tylko, 1989). These categories include history of falling, secondary diagnosis, ambulatory aids, intravenous therapy access, gait, and mental status. Each category is rated on a numerical scale, and the total score helps determine the individual's level of risk for falls.
The Morse Fall Scale is commonly used in hospitals, long-term care facilities, facilities that provide Medicare and Medicaid services, and other healthcare settings to assist in fall prevention strategies. It helps healthcare providers identify patients who may need additional support or interventions to prevent falls from occurring, especially for those who've had fall-related injuries.
In addition to assessing an individual's fall risk, the Morse Fall Scale helps healthcare providers identify specific risk factors that may contribute to falls. Healthcare providers can use this information to develop personalized care plans and interventions for high-risk patients. It also allows for early detection of changes in fall risk, allowing for prompt interventions to prevent falls from occurring.
### **Why should you use it?**
The Morse Fall Scale is a valuable fall risk assessment tool for hospitalized patients, especially in acute care settings. Research by Jewell et al. (2020) showed that the scale could predict falls effectively over a four-month period by identifying risk factors such as gender and specific diagnoses. This enables healthcare professionals to implement tailored interventions, reducing inpatient falls and hospital stays. Do note that this also limits the scale for assessing patients because this is meant to prevent falls in hospitals or similar settings. It would be best to use other similar tools to help you make plans for preventing falls at home and other places.
It helps elderly patients assess fall risk by identifying different risk factors. Bóriková et al. (2018) demonstrated its utility in long-term care settings, where it aids in evaluating fall risk factors among older adults. This targeted approach allows for planning fall prevention strategies and enhancing patient safety and care quality.
The scale is adaptable across various healthcare environments, from hospitals to long-term care facilities. Baek, Piao et al. (2014) emphasized its importance in Korean medical settings for fall-prone patients. Identifying high-risk patients early allows healthcare teams to implement focused nursing interventions promptly.
We recommend that you use other similar assessment tools to examine patients (whether they're a pediatric population or geriatrics), such as the Berg Balance Scale and the Tinetti Balance and Gait Test, to assess a person's ability to maintain dynamic balance, gait, and other factors that may heighten the patient's likelihood of falling.
Add the following tools to your clinical practice's roster of assessment:
- [Tinetti Balance Test](https://www.carepatron.com/templates/tinetti-balance-test)
- [Berg Balance Scale](https://www.carepatron.com/templates/berg-balance-scale)
- [Fall Prevention Checklist](https://www.carepatron.com/templates/fall-prevention-checklist)
- [Fall Prevention Guidelines](https://www.carepatron.com/templates/fall-prevention-guidelines-pdf)
## **How does it work?**
The free Morse Fall Scale Assessment is fully digital and easy to use. You can evaluate your patient using the scale in minutes. Follow these steps to get started:
### **Step 1: Get a copy of the assessment**
Download the Morse Fall Scale using the link on this page. It's available from the Carepatron app or our practice management software's resources library.
### **Step 2: Print or complete digitally**
You can print and complete the assessment by hand or digitally on a tablet or computer. We recommend using digital completion for easier electronic health record-keeping and access.
### **Step 3: Follow the instructions**
The Morse Fall Scale has clear instructions that make it easy to use. Simply follow the instructions and fill in the appropriate scores based on your patient's history, medications, mobility, and mental status.
To fill in the scores, you just need to select the specific answer choice for each item that applies to your patient. The items you need to answer are the following:
- If the patient has a history of falling
- If they have a secondary diagnosis
- If they require ambulatory aids
- If they have IV or IV access
- How is their gait
- What is their mental status
There are fields to the right where you can write down the score per item based on the answer option you picked.
### **Step 4: Calculate the total score**
Once all sections are completed, calculate the total score. This doesn't require anything complex. You can calculate them with the simple method of adding each score per item. The maximum possible numerical score is 125, with a higher score indicating a higher risk of falling. This template doesn't have a Morse Fall Scale calculator, so you'll have to add up the scores yourself, but it does have score ranges with recommended actions.
### **Step 5: Interpret the results**
The Morse Fall Scale includes guidelines for interpreting the total score and determining the patient's risk for falling. This can help with care planning and implementing interventions to prevent falls.
- **A score of 0 - 24** means they have no risk and just need basic nursing care
- **A score of 25 - 45** means they have a low risk or moderate risk of falling and require the implementation of standard fall prevention interventions
- **A score of 46+** means they have a high risk of falling and require the implementation of high-risk fall prevention interventions
Make sure to record the results on your patient's chart to compile all the information you need to help inform other members of your team about the patient's condition, and to inform your treatment plans.
## **Morse Fall Scale scoring guide**
The Morse Fall Scale is a quick and easy-to-use tool for assessing the risk of falls in patients. As mentioned, the scale consists of six items that are scored based on specific criteria (Brigham and Women's Hospital, n.d.):
- **History of falling**: If the patient fell during hospitalization and/or within the past three months, they receive a score of 25 points; otherwise, the score is zero.
- **Secondary diagnosis**: The score is zero if the patient has one active diagnosis or 15 points if they have multiple medical diagnoses for their current admission.
- **Ambulatory aid**: The score is zero if the patient can walk without aids, uses a wheelchair, or is on complete bed rest. The score is 15 if the patient uses crutches or a walker and 30 if they walk while holding furniture for support.
- **Intravenous therapy**: The score is zero if the patient does not have an IV, heparin (saline) lock, or any attached equipment. The score is 20 if the patient has an IV, heparin (saline) lock, or is attached to equipment, such as monitoring equipment or a Foley catheter.
- **Gait**: The score is zero for a patient with a normal gait, walking confidently with head held high, arms swinging freely, and a confident stride. The score is 10 for a patient with a weak gait, slightly stooped, but able to lift their head without losing balance, using furniture as a guide with a light touch, and taking short steps or shuffling. Lastly, a score of 20 is given for a patient with an impaired gait, struggling to rise from a chair, walking with head down, requiring assistance, and having a short, shuffling gait.
- **Mental status**: The score is zero if the patient is fully oriented to time, place, and person. A score of 15 is given if the patient overestimates their abilities, forgets limitations, and has difficulty understanding instructions or responding appropriately.
To calculate the total score, add up the scores from each category. Again, a score of 0-24 indicates no risk for falls, a score of 25-45 indicates low to moderate, and a score of 46 or higher indicates high risk.
It is essential to continually assess fall risk using the Morse Fall Scale throughout a patient's hospital stay, as their risk may change over time due to risk factors such as medication changes, fatigue, or new symptoms.
## **Fall interventions in the hospital**
Since the Morse Fall Scale is meant to assess patients in inpatient or hospital settings, here are some known fall interventions that professionals, especially nurses, can implement to make sure that the patient doesn't fall:
- Have the patient wear footwear that prevents them from slipping because hospital floors might be slippery for some footwear
- Place the patient's call light and their belongings near them so they can easily grab them instead of making an effort to reach too far
- Ensuring proper bed safety is a must. You can do this by locking bed brakes, lowering the bed when they're lying down on it, and raising it when they're about to stand up from it
- Make sure to help them familiarize themself with their room and other parts of the hospital/inpatient setting so they know what they can latch on to in case they need something to hold when your team is not around
- Keep the patient's room clean and uncluttered
These are just some of the interventions you can implement to help reduce a patient's risk of falling and ensure their safety. It's also important that you constantly make rounds and check on the patient.
## **References**
Baek, S., Piao, J., Jin, Y., & Lee, S.-M. (2014). Validity of the Morse Fall Scale implemented in an electronic medical record system. Journal of Clinical Nursing, 23, 2434–2441. https://doi.org/10.1111/jocn.12359
Bóriková, I., Žiaková, K., Tomagová, M., & Záhumenská, J. (2018). The risk of falling among older adults in long-term care: Screening by the Morse Fall Scale. Kontakt, 20(2), e111-e119. https://doi.org/10.1016/j.kontakt.2017.11.006
Brigham and Women's Hospital. (n.d.). Fall TIPS toolkit: Morse fall scale training module [PDF document]. https://www.brighamandwomens.org/assets/BWH/medical-professionals/pdfs/fall-tips-toolkit-mfs-training-module.pdf
Jewell, V. D., Capistran, K., Flecky, K., Qi, Y., & Fellman, S. (2020). Prediction of falls in acute care using the Morse Fall Risk Scale. Occupational Therapy in Health Care, 34(4), 307–319. https://doi.org/10.1080/07380577.2020.1815928
Morse, J. M., Morse, R. M., & Tylko, S. J. (1989). Morse Fall Scale (MFS) [Database record]. APA PsycTests. https://doi.org/10.1037/t24759-000
NHS Inform. (2023, March 14). Causes of falls. NHS Inform. https://www.nhsinform.scot/healthy-living/preventing-falls/causes-of-falls/
World Health Organization. (2021, April 26). Falls. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/falls