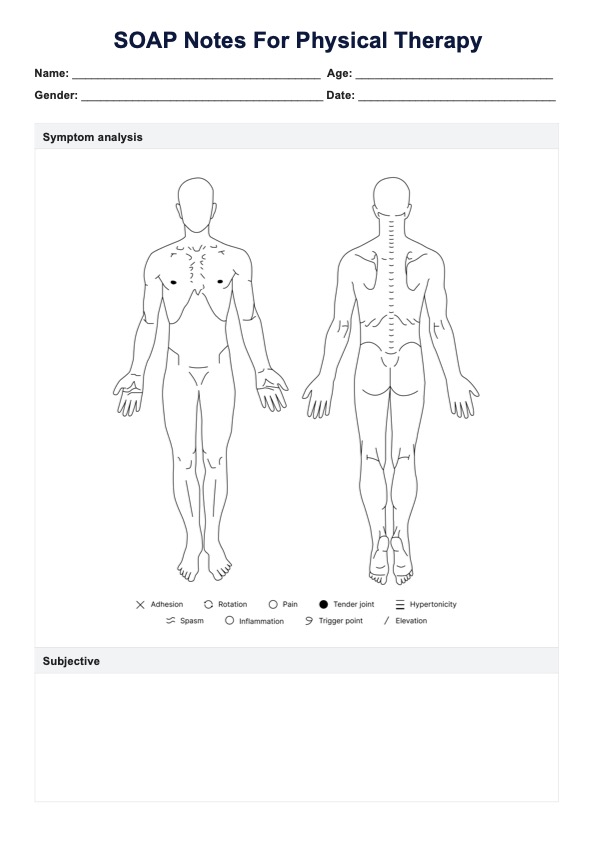
What is a physical therapy SOAP notes template?
Physical therapy SOAP notes are a specific format of progress notes that physical therapists can use to organize their documentation in a consistent and coherent way. Using a PT SOAP note template has many advantages for physical therapists. It helps save time, elevate productivity, and improve clinical outcomes by providing a detailed view of the patient's progress and treatment. You can also find a physical therapy SOAP note PDF to download and use for easy documentation. Sample PT SOAP notes are separated into the four following sections:
- Subjective: The subjective section includes how the patient reports their chief concern (CC). It is ideal to include quotes from the patient, their symptoms, and the patient's functional status.
- Objective: The objective section includes your professional observations about the patient's behavior and affect. You can also include any assessments or tests you completed during the session. For example, this can include vital signs, manual muscle testing, or assessing joint or knee pain.
- Assessment: The assessment is basically a synthesis of the first two sections. You want to state your analysis or interpretation of the subjective and objective sections, indicate how the patient is progressing, and whether the treatment plan appears to be working.
- Plan: The final section of the SOAP note refers to the patient's future treatment plan. This may include upcoming sessions, referrals, treatment plan changes, and goals the patient aims to achieve. For instance, this can include a recommended home exercise program or changes to patient care.
Another resource useful in physical therapy documentation is the Physical Therapy Documentation Sheet, a more guided clinical note specifying each documentation section with respective key components.