AKI Nursing Care Plan
Manage and create effective acute kidney injury nursing care plans through this guide and the easy-to-use and download care plan template!


What is an AKI Nursing Care Plan Template?
Acute Kidney Injury (AKI), or Acute Renal Failure (ARF), refers to a sudden and rapid decline in kidney function, leading to a loss of the organ's ability to filter waste products and excess fluids from the blood. It's a critical condition that can develop within hours or days and often presents in critically ill patients.
AKI can occur due to various reasons, including dehydration, severe infections, medication toxicity, reduced blood flow to the kidneys, or underlying health conditions, and can have a detrimental effect on other organs should it not be treated efficiently and quickly.
In the conventional classification, AKI is typically categorized into three main types. Prerenal AKI is an adaptive reaction to severe volume depletion and low blood pressure, affecting structurally intact nephrons. The second type is Intrinsic AKI, triggered by cytotoxic, ischemic, or inflammatory injuries to the kidney, leading to both structural and functional impairments. Lastly, Postrenal AKI arises due to an obstruction in the urinary passage.
AKI usually requires hospitalization, yet the majority of patients who experience this are usually already hospitalized for other health issues. In serious cases where dialysis is required to assist with kidney functioning, hospitalization may be extended. The focus lies on what is causing AKI rather than the condition itself to effectively treat all symptoms and complications and allow the kidneys to heal.
Patients who have had AKI in the past have an increased risk of developing other health complications or sustaining another AKI in the future. With every kidney injury or renal failure, the chances of developing kidney disease or failure increase.
Instigating an effective nursing care plan that helps prevent the development of other health issues and lowers the chance of redeveloping AKI is paramount. Careful planning and strong foundations in community care and patient education and involvement is key.
AKI Nursing Care Plan Template
AKI Nursing Care Plan Example
How does it work?
Step One: Gather your resources
AKI nursing care plans are a valuable resource and essential to keep on hand. Make sure that you have a copy of the free printable PDF when the need arises by either clicking the “Download Template” or “Use Template” button or by searching “AKI nursing care plan” on Carepatron’s template library’s search bar on the website or app.
Step Two: Collate essential information
Once the patient has been diagnosed and assessed for a decrease in kidney function, utilizing the AKI nursing care plan template to ensure all goals of care are met is both seamless and easily accessible to relevant parties via Carepatron's centralized workspace.
Assessment, symptom management, and interventions can be collated within the single care plan and safely stored on a single database. The care plan allows for individualized treatment options. It acts as a scaffolding to ensure goals of care are met, and the next steps are recorded for future reference or distribution to other healthcare specialists who are part of the patient's care team.
Step Three: Store the chart securely
After reviewing the AKI nursing care plan and creating a viable and individualized plan for the patient, you need to secure the plan so that access is only granted to relevant parties.
Ensure this through Carepatrons HIPAA-compliant free patient records software. Here, all relevant medical records can be safely stored and collated for ease and security.
When would you use this template?
An AKI nursing care plan can be utilized when a patient is diagnosed with or at risk of developing AKI. AKI refers to a sudden and rapid decline in kidney function, often caused by various factors such as dehydration, severe infection, medication toxicity, or reduced blood flow to the kidneys due to trauma or surgery.
A care plan is essential in managing and addressing the specific needs of patients experiencing or at risk of AKI. Some scenarios where an AKI nursing care plan can be used include:
Hospitalized patients
Individuals admitted to hospitals due to conditions that predispose them to AKI, such as severe infections, heart failure, sepsis, or after surgeries where there's a risk of kidney injury.
Critical care units
Patients in critical care units, particularly those with conditions that can lead to AKI, require close monitoring and tailored interventions to prevent kidney damage or manage existing AKI.
Chronic disease management
Patients with chronic conditions like diabetes or hypertension, which can contribute to kidney damage and AKI, may require ongoing care plans to prevent acute episodes.
Medication management
Some medications, such as certain antibiotics or contrast dyes used in imaging tests, can cause kidney injury. Patients receiving these medications may need a nursing care plan focused on preventing AKI.
What do the results mean?
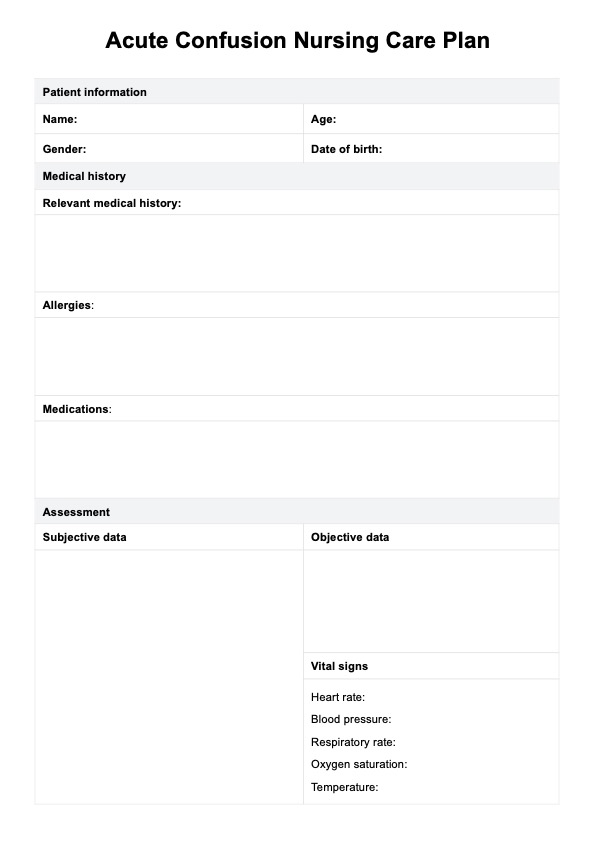
Assessment
Assessing for signs and symptoms of Acute Kidney Injury (AKI) involves observing both subjective and objective indicators, some of which may include:
- Physical signs: Reduced urine output (oliguria), swelling in hands, feet, or face (edema), fatigue, weakness, and shortness of breath.
- Gastrointestinal symptoms: Nausea, vomiting, loss of appetite, abdominal pain, or discomfort.
- Neurological signs: Confusion, altered mental status.
- Cardiovascular manifestations: Elevated blood pressure, irregular heart rhythm, palpitations, and signs of fluid overload.
- Renal factors: Compromised regulatory mechanisms leading to kidney failure, fluid overload due to kidney dysfunction or excessive fluid replacement, and electrolyte imbalances like potassium or calcium irregularities.
- Metabolic effects: Acidosis, uremic effects on cardiac muscle, increased metabolic needs, and protein catabolism.
- Secondary issues: Gastrointestinal symptoms impacting dietary intake, immunological defense depression due to uremia, invasive procedures/devices like urinary catheters, dietary changes leading to malnutrition, and diuretic phases contributing to excessive fluid loss.
Interventions
Nursing interventions for Acute Kidney Injury (AKI) focus on addressing the underlying causes, preventing complications, and supporting kidney function. Interventions include, but are not limited to:
- Fluid management: Monitoring fluid intake and output, adjusting fluid therapy as needed. Regulating fluid balance prevents complications like fluid overload or dehydration, which is crucial in maintaining kidney function.
- Electrolyte management: Monitoring and managing electrolyte imbalances (e.g., potassium, calcium). Correcting electrolyte abnormalities helps prevent cardiac irregularities and supports cellular function.
- Medication management: Administering medications as prescribed, adjusting doses based on kidney function. Medications must be carefully managed, as some drugs can exacerbate kidney damage or require dose adjustments due to impaired renal function.
- Nutritional support: Collaborating with dietitians to create an appropriate diet plan.
A balanced diet helps manage electrolyte imbalances, reduces the workload on the kidneys, and supports overall health.
- Vital signs monitoring: Regularly monitoring vital signs, including blood pressure and heart rate. Early detection of changes in vital signs allows for prompt intervention and prevention of complications like fluid overload or cardiovascular issues.
- Education and support: Educating patients and families about AKI, medications, dietary restrictions, and the importance of follow-up care. Empowering patients with knowledge enables better self-management, adherence to treatment plans, and prevention of recurrent AKI episodes.
- Prevention of complications: Preventing infections, and monitoring for signs of complications like fluid overload or sepsis. Early identification and management of complications contribute to better outcomes and prevent further kidney damage.
- Collaboration with healthcare team: Collaborating with physicians, nephrologists, pharmacists, and other healthcare professionals. Multidisciplinary collaboration ensures comprehensive care, addressing various aspects of AKI and its management.
Research & evidence
Acute kidney injury represents a significant challenge for acutely unwell patients, carrying substantial risks of mortality and illness globally (Chawla et al., 2014). This condition can be pre-existing before hospital admission or arise during hospitalization and according to the Kidney Disease Improving Global Outcomes (KDIGO) report, the occurrence of acute kidney injury among hospitalized individuals ranges from 17% to 31% (Bedford et al., 2014; Susantitaphong et al., 2013).
Managing acute kidney injury during hospital stays leads to escalated healthcare expenses as a result of prolonged hospitalizations, additional tests, and the emergence of complications such as the necessity for renal replacement therapy (RRT), cardiovascular issues, and readmissions (Chertow et al., 2005).
A 2009 National Confidential Enquiry into Patient Outcomes and Death (NCEPOD) highlighted that 50% of AKI-related deaths involved subpar care, and 14% of AKI cases were preventable (sterwart et al., 2009). The International Society of Nephrology initiated the 0by25 program in 2013, aiming to enhance prompt diagnosis and treatment of acute kidney injury worldwide, seeking to eliminate avoidable AKI-related deaths by 2025 (Mehta et al., 2015). Research and evidence such as this report further highlights the importance and need for easily accessed and well-utilized nursing care plans.
Initially viewed as a completely reversible condition, AKI is presently acknowledged as a contributor to chronic kidney disease (Basile et al., 2001). This risk remains even after serum creatinine (SCr) levels return to normal following the acute phase (Lo et al., 2009). Individuals needing dialysis due to CKD experience a changed health-related quality of life (HRQOL), and renal replacement therapy (RRT) presents a significant financial burden on healthcare systems (Elshahat et al., 2020). Work is also being done to investigate the long-term survival of those who have suffered from AKI (Hobson et al., 2009).
References
Basile, D. P., Donohoe, D., Roethe, K., & Osborn, J. L. (2001). Renal ischemic injury results in permanent damage to peritubular capillaries and influences long-term function. American Journal of Physiology-Renal Physiology, 281(5), F887–F899. https://doi.org/10.1152/ajprenal.00050.2001
Bedford, M., Stevens, P. E., Wheeler, T. W., & Farmer, C. K. (2014). What is the real impact of acute kidney injury? BMC Nephrology, 15(1). https://doi.org/10.1186/1471-2369-15-95
Chawla, L. S., Eggers, P. W., Star, R. A., & Kimmel, P. L. (2014). Acute kidney injury and chronic kidney disease as interconnected syndromes. The New England Journal of Medicine, 371(1), 58–66. https://doi.org/10.1056/NEJMra1214243
Chertow, G., Burdick, E., Honour, M., Bonventre, J., & Bates, D. (2005). Acute Kidney Injury, Mortality, Length of Stay, and Costs in Hospitalized Patients. Journal of the American Society of Nephrology, 16(11), 3365–3370. https://journals.lww.com/jasn/fulltext/2005/11000/acute_kidney_injury
Elshahat, S., Cockwell, P., Maxwell, A. P., Griffin, M., O’Brien, T., & O’Neill, C. (2020). The impact of chronic kidney disease on developed countries from a health economics perspective: A systematic scoping review. PLOS ONE, 15(3), e0230512. https://doi.org/10.1371/journal.pone.0230512
Hobson, C. E., Yavas, S., Segal, M. S., Schold, J. D., Tribble, C. G., Layon, A. J., & Bihorac, A. (2009). Acute Kidney Injury Is Associated With Increased Long-Term Mortality After Cardiothoracic Surgery. Circulation, 119(18), 2444–2453. https://doi.org/10.1161/circulationaha.108.800011
Lo, L. J., Go, A. S., Chertow, G. M., McCulloch, C. E., Fan, D., Ordoñez, J. D., & Hsu, C. (2009). Dialysis-requiring acute renal failure increases the risk of progressive chronic kidney disease. Kidney International, 76(8), 893–899. https://doi.org/10.1038/ki.2009.289
Mehta, R. L., Cerdá, J., Burdmann, E. A., Tonelli, M., García-García, G., Jha, V., Susantitaphong, P., Rocco, M., Vanholder, R., Sever, M. S., Cruz, D., Jaber, B., Lameire, N. H., Lombardi, R., Lewington, A., Feehally, J., Finkelstein, F., Levin, N., Pannu, N., & Thomas, B. (2015). International Society of Nephrology’s 0by25 initiative for acute kidney injury (zero preventable deaths by 2025): a human rights case for nephrology. The Lancet, 385(9987), 2616–2643. https://doi.org/10.1016/s0140-6736(15)60126-x
Sterwart, J., Findlay, G., Smith, N., Kelly, K., & Mason, M. (2009). Acute kidney injury: adding insult to injury. Natl Confid Enq into Patient Outcomes Death. Susantitaphong, P., Cruz, D. N., Cerda, J., Abulfaraj, M., Alqahtani, F., Koulouridis, I., & Jaber, B. L. (2013). World Incidence of AKI: A Meta-Analysis. Clinical Journal of the American Society of Nephrology, 8(9), 1482–1493. https://doi.org/10.2215/cjn.00710113
Commonly asked questions
To create a comprehensive nursing care plan for AKI management, simply create a customized plan from the scaffolding provided by Carepatron and cater to the patient's needs through the key aspects of assessment, diagnosis, planning, intervention, and evaluation.
These valuable plan templates can be used at any point of the treatment journey for a patient who has had an acute kidney injury to track, monitor, and plan all interventions both by healthcare professionals and the patient themselves.
AKI nursing care plan templates are used to plan efficient and confident care delivery. They are designed to be customized to meet the individual patient's needs.